The Original Beginner's Guide to FD
What is Feline Diabetes, and How Does it Affect My Pet's Health?
Diabetes is a disorder affecting the processing of glucose (blood sugar) in the body. The digestive system breaks food down into various components, including glucose, that enter the bloodstream. Glucose is absorbed by cells to use for energy. Insulin is the hormone that signals the cells to take up the glucose — without it, the glucose stays in the blood. A VERY simplified diagram is presented below to help explain this process.
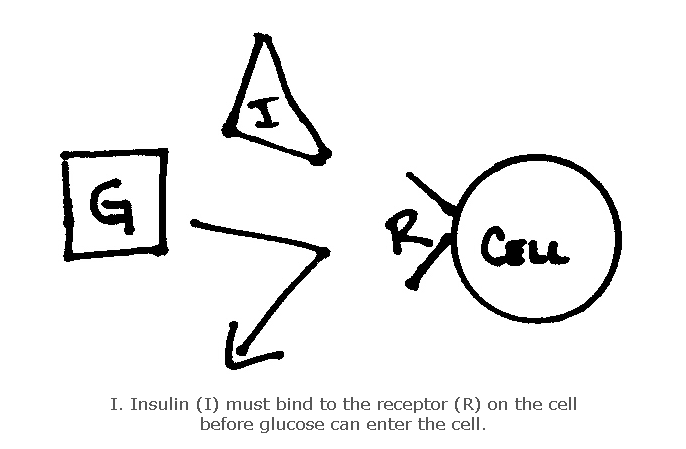
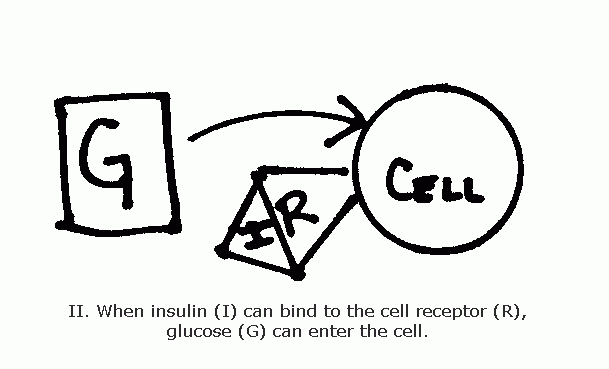
In a normal digestive system, the arrival of food stimulates the organ called the pancreas to secrete insulin into the bloodstream to regulate glucose levels. More food, more insulin. More insulin, less glucose in the blood (and more in cells to use for energy). At its simplest, diabetes is a disorder of this process. If there isn’t enough insulin or if insulin can’t act properly on cells, the glucose level in the blood stays too high and the glucose is not available for the cells to use as energy.
Diabetes is generally divided into two different types, Type I and Type II. Type I (which is also sometimes called juvenile diabetes or Insulin Dependent Diabetes) occurs when the pancreas doesn’t produce enough insulin. Looking back at the simplified diagrams, taking away the insulin removes the “key” that binds to the cell receptor (“the lock”) and lets the insulin “through the door” into the cell. When this happens, glucose levels stay high in the bloodstream and the cell lacks enough glucose for its energy needs.Type II diabetes (sometimes referred to as adult onset diabetes or non-insulin dependent diabetes) occurs when there is a problem with the receptor or “lock.” The “key” (insulin) won’t fit into the lock and so glucose once again cannot get into the cell and high blood sugar, called hyperglycemia, results.
The pancreas may malfunction and not make insulin, or enough insulin, due to a number of factors. The pancreas can be damaged by an infection or inflammation, steroid medications may affect it, and dietary deficiencies may even play a role. There also seems to be a genetic predisposition to pancreatic malfunction in some cases but no particular breeds of cats seem to have this. Some of the damage diabetes does to the body is due to the glucose staying in the blood but a lot is due to the fact that for lack of glucose, the cells malfunction. The body begins to die of starvation because cells cannot reproduce themselves when their life span is complete (a matter of weeks).
Diabetes is sometimes diagnosed as the result of a routine blood test and the luckiest cats are treated before symptoms show up. Most are diagnosed because the owner noticed one or more of the primary signs:
- PU or PD (abbreviated PU/PD):
- PU=polyuria = frequent or excessive urination
- PD=polydipsia = frequent or excessive drinking
- Weight loss despite eating well
The diabetic is hungry, eats more, but loses weight anyway. Some organs will attempt to correct the problem — the kidneys, for instance, try to get rid of the excess glucose in the blood and go into high gear. They use a lot of water for this, so the diabetic feels thirsty all the time and drinks a lot of water (polydipsia or PD), and urinates huge amounts of dilute urine with sugar in it (polyurination or PU. You will probably hear this renal (kidney) affect called “spilling glucose.” Because of this extra effort, the kidneys are usually among the first organs to show damage from diabetes but this damage usually isn’t evident until quite advanced. Eye and nerve damage tend to be noticed first. If there is damage at the time of diagnosis, the diabetes has been there for quite a while and has gotten severe.
Diabetes, although relatively simple in concept, turns out to be extremely complex and variable in practice. Additionally, diabetes in cats is not a deeply studied subject. Because of this, some veterinarians still resist treating feline diabetes or don’t have appropriate information. Sadly, there are still an ingorant few who don’t recommend that treatment be attempted. Fortunately, most veterinarians are open to education, even by cat caretakers. Keep in mind that veterinarian guidelines for treating feline diabetes are based on average results achieved with large numbers of animals. It’s rare for an individual animal to fit nicely into that picture, so either you or the vet has to learn a lot about diabetes in YOUR cat so that your pet can be treated effectively and live many more happy years.
The object of diabetes treatment is to control the blood glucose so it stays in (or near) the normal range, as it would be if the pancreas were still producing insulin naturally. For food to be properly utilized, insulin must be available to convert the food into a useable state. The pancreas would naturally regulate blood sugars by slowly releasing insulin, and unfortunately injected insulin doesn’t act quite like natural insulin, nor is it practical to just shoot a little in every time the cat eats.
You need to consider additional ways to help control your cat’s blood sugar. Diet is the most important part of treatment and some cats can actually be diet-controlled. Although many vets are not aware of it, current research indicates that a high protein, low carbohydrate diet is best for cats. Since cats are obligate carnivores, they don’t have the proper enzymes to digest plant-based protein, so avoid any foods that use plants as the primary protein source. For choosing the best food for your cat, you can review some excellent articles on this type of diet in the Health Articles section of this site.
If diet alone does not control the diabetes, your cat will need medication, either insulin or an oral antihyperglycemics (pills). If you opt to try pills, research indicates that it can take up to four months before a cat begins to respond to them. Depending on your cat’s overall health at diagnosis, you may not want to wait this long. Also, most cats don’t seem to respond to the pills so injected insulin may be the best treatment option. Several types of insulins with different characteristics are available to use, as not all cats react the same way to each type. Humulin N has a very poor history of working correctly on cats and should be avoided. Non-human insulin such as pork or beef PZI is closest to the structure of a cat’s own insulin. Again, the Health Articles section has a number of articles on insulin.
If your cat is newly diagnosed with diabetes but is not severely ill, you should consider taking your cat home, learning to do home blood-testing with a simple glucose meter, and get your cat’s diabetes under control at home with your vet’s guidance. Veterinarians will choose an insulin and an initial insulin dosage based on treatment guidelines. Your vet will tell you if your cat is too sick to go home. If he has complications, your cat will have to stay in the hospital until he gets well enough to treat at home. If you feel that you cannot do glucometer testing, at least test your cat’s urine with simple dipsticks.
Diabetes can be permanent or temporary, stable or variable, or even intermittent — it’s called a “honeymoon” when the diabetes disappears briefly.
Deciding Whether to Treat is a Difficult Decision, but the Resources are Here
Diabetes is complex, and trying to understand it all in one big gulp won’t work. Once you’ve made the decision to be a diabetic’s caregiver, focus on one thing at a time — follow your vet’s advice and get the basics straight in your head. Doubt everyone; lots of people will give you good advice, but no one thing works for every diabetic, and no one technique works for every owner. Sometimes even the vet’s advice may seem unclear or even wrong. Always question what you don’t understand.
As you learn more, keep going back and reviewing the things you already know and fitting the new stuff into the “big picture.” The big picture is different for everybody, and you have to create your own. Study everything you can get your hands on, both veterinary and human. Pick up brochures at vets and pharmacies and hospital metabolic centers, take out library books, cruise the internet. Ask questions of everyone — the vets, nurses and doctors, human diabetics, other owners of diabetic animals. Ask the same questions of many people, because you will get widely disparate answers and have to choose for yourself which one you believe.
Plenty of support exists for you. The MUFFIN email list is a jewel, and the Feline Diabetes Message Board (FDMB) will connect you with a whole community of people who have diabetic cats and will give you almost immediate feedback. The only thing we have all agreed on entirely is this: trust your own good sense. IF YOU THINK SOMETHING IS NOT RIGHT, TRUST YOUR SELF. A cat’s wellness is broadcast by a constellation of behaviors, and the only one who knows him well enough to get the message early is you, who lives with him and cares enough to observe closely and thoughtfully.
Insulin
Insulin is somewhat delicate, and opinions differ on just how delicate. Generally, avoid extremes of temperature, especially freezing, as this will render the insulin inactive. Be sure to review the manufacturer’s recommendations for storage and for expiration dates. Different types of insulin will often have different storage requirements and stability. Some must be kept cold, some at room temperature, and it is best to keep them away from light/
Vigorous shaking is bad. The insulin is a fine powder that doesn’t dissolve in the diluent (the liquid) — it’s just suspended in it. When it’s shaken a lot of air bubbles form: the big ones are easy to see and deal with, but the microscopic ones are harmful. They allow the insulin particles to be in contact with air, which degrades them, and the total volume of air in those bubbles changes the dosage in the syringe. Also, vigorous shaking can actually denature the protein, meaning that the insulin molecule is broken up and won’t function properly. The insulin bottle will get some shaking in transport, so when you get it home let it settle in the fridge several hours.
Mix the insulin thoroughly every single time you use it. Roll the vial between your hands, tipping it a little up and a little down as you go. Or gently turn it upside down several times. Most insulin should look evenly cloudy if mixed properly. Again, note what the new bottle looks like because some forms of insulin will look differently. If you draw a single dose out of a vial that wasn’t uniformly mixed, the strength of the suspension remaining in the vial is changed. If you drew out too much insulin one time, the vial will contain a weaker solution: if you drew out too much diluent just once, the rest of the insulin is too strong. Don’t get too panicky about this. Just mix it thoroughly and gently and you will be fine.
Some insulins settle out of the diluent very fast, so don’t let the vial rest after you’ve mixed it — have the syringe ready. It doesn’t matter if it rests a while in the syringe, since it’s all going to be injected anyway. If you have to store a filled syringe for long (for instance, leaving it for someone else to inject) store it needle-up so the needle doesn’t dry and clog up.
Different types of insulin used vary on how they are made and how long they act in the body. There are also different names depending on the manufacturer. The most common type of insulin used in cats is used to be Humulin (human-based) but there are other types used, too. All insulins are measured in units, but they do not directly compare to each other. Six units of PZI is not the same as six units of Humulin or Caninsulin. Common terms are “regular” (fairly fast-acting), “lente” (slow-acting), and “ultralente” (very slow-acting). Insulin is shipped with a pamphlet describing it’s characteristics (or “profile”) and your pharmacist will probably include a copy.
Some insulins come from the manufacturer in ready-to-use vials, some are sold as powder that the vet or pharmacist mixes with special diluent (or sometimes ordinary saline solution) according to your needs. A vet who compounds in his office can vary the strength for you — if you’re giving huge doses, he can make it stronger so there is less discomfort for the cat; if you’re having trouble with dosage accuracy, he can make it weaker and eliminate the need for measuring half or quarter units.
Insulin is made from various sources — beef and pork are common in veterinary insulins, although many vets prescribe human insulin.
Insulin doesn’t keep forever and you may find that it gets less effective as you near the bottom of the vial — always start a new vial on a weekend or a day when you’re able to stay home with the cat, in case the new batch is stronger. Opinions vary widely about how well insulin keeps. Some people say you should throw it out after 30 days, or making 30 draws. Others say it’s fine to the bottom of the vial even if that means three months and a hundred draws. I say just keep a sharp eye on the appearance of the contents, keep the stopper clean, and be vigilant for signs of reduced strength by monitoring the cat.
If possible, have a spare vial on hand — if you drop your only vial and it breaks, it’s sure to happen on Friday night. One way to do this is to save the last part of a vial before starting a new vial. When you get almost through with the new vial, save the last of it and throw away the old vial. Another reason to keep extra in the fridge is so you can immediately switch vials if you notice that the solids in the vial have clumped and won’t dissolve, or see contaminant particles, or notice anything strange about the suspension.
If you forget to give the insulin at the appointed time, it’s better to skip it altogether. If you’re only an hour or two late, you can give the shot, but you have to reschedule subsequent shots. To move the cat back to his regular time, advance each injection by no more than half an hour.
Syringes
Human insulins are “U-100” — there are 100 units of insulin in each cubic centimeter (or millilitre). Some veterinary insulins are U-40 (40 units/cc). You should have the correct syringes for the prescribed insulin — a U-100 syringe will measure the exact amount of U-100 solution to ensure that the right number of insulin units are administered.
If you wish to use U-100 syringes with U-40 insulin, you have to calculate the volume needed to administer the correct number of units. It’s safer to make a chart so you don’t have to risk a dosage error by doing calculations in your head when you might be too tired to think straight The conversion factor is 2.5. FelineDiabetes.com has a conversion chart for reference and printing if you wish to use U-100 syringes with a U-40 insulin.
Syringes will be cheaper if you buy them by the carton, containing 100 syringes. Prices vary widely according to brand and to store. Check around. Cats are usually on smallish dosages, so the small-capacity (3/10 cc) syringes work well, with the added bonus of having the gradation marks further apart and easier to see.
Syringes are pretty cheap, so use them only once. If you absolutely must reuse the syringe, use it twice at most. Needle tips quickly degrade, and become uncomfortable after only one or two uses.
The needles on insulin syringes vary from very fine to extremely fine, and bend easily. Never try to straighten a bent needle. If your hands are unsteady or you have trouble injecting, you might want to start with a larger, stiffer needle. You can try finer ones later (some makers offer free samples through drugstores). The amount of pain the cat feels from the stick is minimal, so larger needles don’t make a noticeable difference to the victim.
If you do use a larger, stiffer needle, be aware that you can stick yourself more easily. Don’t worry, although you will hurt, you won’t get diabetes or any other illness. Just wash your hands and apply some pressure to stop the bleeding. Needles have gotten better in the last few years. A lot of people are now using ultrafine 30-gauge (30 g), extra short needles that the cat barely notices.
Never use a needle that has been in contact with anything except the vial stopper. If it touches the table or your fingers, throw it away, insulin and all if necessary. Don’t try cleaning these needles — the outside has a teflon-like coating that makes it slip in easier, and cleaning removes this coating (and the tiny hole in it would still be dirty, or coated with whatever you tried to clean with).
If you re-cap a syringe (not recommended), be sure to hold one hand still and move just the other one. If both hands are moving you might not go in straight, and the needle will come out the side of the cap and stick your finger. Small needle clippers are available to clip off and store the needle. The syringe then can be thrown away. If you don’t use a needle clipper, use a container called a “sharps” box to put the uncapped needle and syringe into. Sharps containers are widely available or you can make your own using a plastic milk jug or soft drink bottle. Many county disposals will take full sharps containers at no charge.
Injections
The injection site influences how insulin works. If it goes straight into the bloodstream, you have an almost instant overdose. If it goes into a slab of fat, it will take forever to get to the blood for distribution to the rest of the body. Muscle is good, but painful for the cat, and hits the bloodstream pretty fast. You want it to go under the skin (“subcutaneous” or “sub-Q” or “SQ”) in an area where there is good circulation and the only discomfort is a tiny prick.
You can inject anyplace that works for you, but the scruff of the neck should be avoided due to its poor blood supply. Either side of the spine, between the scruff and the hips, and at least an inch away from the backbone, is also good and along the abdomen is excellent. If you use an alcohol swab to clean the top of the vial, make sure the alcohol has completely dried before sticking the needle through. It isn’t necessary to swab alcohol on the the injection site. If your cat has long hair and you are inexperienced with giving injections, you might trim a little hair in several spots to help you visualize the skin. Try to rotate injection sites to help prevent the formation of “granulomas” that are small knots of tissue with very poor blood supply.
To fill a syringe, pull back the plunger to the mark corresponding to the dose you want to give. After gently mixing the insulin, turn the vial upside down, insert the syringe into the vial stopper and inject the air completely. Keeping the vial upside down and the syringe nearly vertical, fill the syringe. When you fill the syringe, don’t pull the plunger too fast — that will cause microbubbles. Gently and slowly pull the plunger back to the desired dose mark. Tap the syringe while it’s still in the vial to move air to the top, and squeeze the air back into the vial before measuring. Your finger, the back of a paring knife or a pencil can be used for tapping.Always measure the same way — hold the needle in the same position, and set the plunger at the same place relative to the mark on the barrel.
Put the insulin back in the fridge right away to stay cold although most insulins won’t be harmed if they are left at room temperature for a few hours. If you like, you can hold the filled syringe in your hand for a minute or two to take the chill off, or let it come to room temperature while you get the meal ready.
You can very your timing and approach to injection to suit your cat. Injecting while the cat is eating and his attention diverted works for many cats. The syringe barrel is held between two fingers and the plunger depressed with a third finger. Some people hold the syringe between the index and middle fingers, with the thumb ready to depress the plunger once the needle has entered the skin. Others hold the syringe between their thumb and middle fingers so the index finger is available to push the plunger. Don’t put your finger on the plunger until you are ready to inject to avoid injecting into the fur only. Turn your hand over so the syringe is between your hand and the cat, which ensures that the needle is almost parallel to his body. The needle gets jabbed sharply into the skin, about halfway up the tent of skin. Many people will then pull back on the plunger slightly to make sure the needle isn’t in a blood vessel. This is awkward for a beginner and if you are careful about only pulling up the skin and subcutaneous tissue, it should be unnecessary. Make sure your veterinarian demonstrates how to give shots and then watches your technique. You can practice on a piece of heavy vinyl, a pickled pig’s foot, or many other objects until your movements are smooth.
Always stroke the injection site afterward — if you feel moisture, then you lost some of the insulin. If you can’t be there to watch for hypoglycemia later, never give additional insulin. Just note on your injection chart that your cat’s dose went short by an unknown amount. It can be helpful to post a schedule on the refrigerator so you can check off when shots are given. This is especially important when more than one person in the household may give the shot.
Monitoring
Monitoring is a permanent necessity, since diabetes is quite variable in its effects. In the early weeks, you monitor to see if enough insulin is being given. Once that’s accomplished, you monitor to ensure that the insulin needs haven’t changed.
There are four main ways of monitoring, each providing various levels of accuracy. The method you choose should be the one you are most comfortable with doing. Although even home testing can be easily learned and we feel it is the best method, every caretaker must decide for themselves. Caretakers of diabetic cats should also be cautious in not criticizing those who do not opt for their method of monitoring.
1. PU/PD
The grossest measure (in terms of accuracy as well as sensibility) is PU/PD — you simply observe drinking and urinating. An out-of-control cat will be at the water dish frequently, and flooding the litter box. Almost any amount of insulin will reduce PU/PD, but all you really know is that there is an improvement … no telling how much, and when you’ve gone too far you find out the hard way when the cat has an insulin reaction.
You can get an idea of how much your cat drinks by measuring the water that is put out, and after 12 hours, measure how much is left. A normal cat will drink four ounces in 12 hours. See the FAQ section of the Feline Diabetes web site for more measurements.
2. DIPSTICKS
The next best monitoring method is urine testing with reagent strips, or “dipsticks.” These are available at drugstores as human testing devices … none are made for cats specifically. There is controversy over whether these really are useful. Some vets say there’s no point, since nobody has bothered to find out whether cat urine is similar enough to human urine to make the readings reliable. Many people are monitoring solely with dipsticks, and very happy with the results. Please read the FAQ on Adjusting Insulin Dosages Using Urine Strip Results for some further information. Proceed with great caution if you want to make dose changes based on urine strips alone.
Read and follow the “care and keeping” instructions on the container, and if you get odd results buy a new batch of dipsticks.
There are as many ways of collecting urine samples as there are cat/owner teams. Some just hold the stick in the urine stream, if necessary pulling up a bit on the tail to get a look at where you’re sticking your hand. Or you can clip the dipstick onto a reacher of some kind. Or stick a large spoon under him. If you can’t catch the cat in the act, or he won’t pee with you hanging over, you can isolate him with a litter box containing a few pieces of shredded newspaper or some well-rinsed aquarium gravel and dip the stick in the puddle.
When a diabetic’s blood glucose gets close to 200 mg/dL, the kidneys start flushing out the excess and it winds up in (or spills into) the urine. The dipsticks change color according to how much glucose is in the sample, but the reading is far from precise, so it must be done several times in each insulin cycle until the cat is regulated, and occasionally thereafter.
A normal cat will never have the slightest trace of glucose in his urine. An uncontrolled diabetic will have very large amounts. The difficulty with reliance on urine testing is that when you test, you’re looking at the previous several hours of glucose levels — the kidneys take some time to gather the glucose, and it collects for some time in the bladder. If you see a high glucose reading, you have no way of knowing if the blood levels were high for the entire time, or if there was a brief spike five hours ago.
Those who use urine monitoring like to see a trace of urine just before an insulin injection is due, and none at all in the rest of the samples. The trace at the beginning of the cycle means that the BG (blood glucose) went a little high as the insulin effect tailed off, which is interpreted to mean the cat isn’t being overdosed on insulin and it’s safe to give the next shot. The negative readings mean the blood glucose was below the renal threshhold during the previous few hours.
3. BLOOD TESTS
The most timely and accurate monitoring is blood testing. You can know with certainty what the cat’s blood glucose is at the time of testing.
a. Testing at the Vet
This is the route a lot of people take when they don’t feel comfortable with home blood tests. It can get expensive as you will normally pay an office visit charge and then a fee for a “spot” (individual) blood test or a fee for a “glucose curve” (a series of blood tests). As mentioned before, stress can affect these tests, especially the spot tests. If you decide to do home testing, occasional visits to the vet are still recommended to check kidney function, do long-term tests like fructosamine (see below), and for general checkups. Many cats are managed well with this routine.
b. Home Blood Testing
This is the most difficult (but easily learned!), in that obtaining samples involves pricking the skin somewhere to obtain a drop of blood. This method is less expensive while ensuring excellent monitoring. Blood testing can range from the occasional check to confirm your suspicion of hypoglycemia, to taking full control of regulating the cat’s diabetes and doing glucose curves.
Glucometers made for human diabetics are used, and provide sufficient accuracy for optimal blood glucose control. These meters are very accurate in the normal ranges, less so as the the glucose levels approach extremes. This doesn’t matter, since all you need to know is that an extreme has been reached — the extent of the extreme is less important than the fact that the glucose is far from where you want it.
A frightened or angry cat’s blood glucose will spike — this is the normal physiological response to stress, providing a sudden burst of glucose for extra energy to run or fight with. In a normal cat, this is accompanied by a burst of insulin so the glucose can be used by the muscles and other tissues. In a diabetic, it goes into the blood and stays there. The glucose spike can be anywhere from 50 to several hundred mg/dL. The implications for blood testing are considerable — if you took the cat to the vet for blood tests, he has been stressed by the car ride and the waiting room, and may go totally nuts when he’s grabbed for yet another painful and humiliating procedure. Even if the cat seems calm, you should allow for some stress elevation when blood glucose tests are done — a larger elevation if done by the vet, less if done at home.
In cats, the ear is generally the best site for blood testing. Although sensitive to touch, it is a relatively insensitive area to prick (lancets cause less pain than a mosquito bite). A paw pad can be used, but since the paws are on the floor and in the litter box, more care has to be taken about keeping the little puncture wound clean to avoid infection. Some people use an insulin syringe to draw a little blood from a leg vein — I haven’t had to resort to this and cannot comment on it at all. Unless you have medical training and know how to properly restrain a cat, this method is best left to professionals.
There are several detailed procedures on how to do ear sticks posted under Home Blood Glucose Testing of the Diabetic Cat so I won’t repeat any of it here. Each person has to develop their own way of getting the sample from their own cat.
If your glucometer reads in mmol/L, multiply by 18 to get mg/dL. There is also a blood glucose unit converter calculator on this site so you can plug in values to get a conversion.
c. LONG TERM TESTS
The vets can do blood tests (fructosamine, glycosylated hemoglobin) that show how well the diabetes has been controlled over a long period (weeks) of time. These tests are based on the fact that certain blood components are affected by high levels of glucose, and these components only live for a few weeks. If they are normal, you assume the diabetes has been well controlled during the entire lifetime of those cells. If they are changed, then you know that the diabetes was out of control for some or all of that time.
These tests are not very helpful for getting a cat regulated, but very good for periodic checking of ongoing control in a regulated cat since they completely eliminate the stress factor. Consider having your cat tested in this manner at least once a year.
Regulating
As soon as diabetes is diagnosed, it is important that sufficient insulin be given to bring the glucose levels down closer to normal ranges. Every day, every hour, of high blood glucose is damaging the cat, and some of that damage is irreversible.
How aggressive should you be with increasing insulin dosages? That is a judgement call, and one that vets and caretakers differ on widely. Some vets will have 24-hour staff and be able to take the cat for several days and get him regulated. They will increase the insulin by one or two units every 12 hours, monitor the glucose levels every hour or two around the clock, treat hypoglycemia if it happens, and establish a feeding schedule that suits the action profile of the insulin they chose. Some vets will go to the other extreme, selecting an insulin and a starting dosage, advising on insulin and feeding schedules, and leave it up to you to bring the cat back if symptoms don’t improve. Most vets are somewhere in between, getting you started on a schedule and asking to have the cat brought in at weekly or semi-weekly intervals for blood tests. This can take months if the increments are small and the intervals long, during which time the cat suffers more and more organic breakdown. Plus, if it turns out the cat doesn’t respond well to the first insulin, the whole drawn-out procedure is begun again for a new insulin. I believe that while this approach sometimes works, and is comfortable for both the owner and the vet, it is excessively conservative. The individual caretaker must decide what is best for the cat and the responsive vet will understand. I strongly advocate aggressive regulation by the owner, with the vet involved every step of the way — if he’s made of the right stuff, he’ll work with you and support your efforts with advice and information. Otherwise you may have to look at getting a new vet, educating your current vet (see Spread the Word), or finding a specialist to deal with just the diabetes. In the worst case scenario you’re out there all alone except for your community on the Feline Diabetes Message Board.
Regulating your cat ideally requires an understanding of how insulin works, and the relationship between insulin and food. It requires patience, and a certain scientific detachment to overcome the instinct to make several changes simultaneously in a desperate attempt to stumble on something that works. Even if you get lucky and find that the glucose is under control, you won’t know why, and when something changes (and it will) you have no knowledge to help you decide on how to deal with the sudden loss of regulation.
One simplistic approach is to increase insulin slowly until you think the cat feels pretty good. For me that is just the starting point. I believe that blood testing is the sole reliable measure of regulation — the brain grabs it’s share of the available glucose, if necessary short-changing the body cells … the cat may be perkier and more responsive, but some organs are left in a permanent state of minor overload, and the rest of the tissues slowly deteriorate.
“Normalization” is the term used when the control is perfect and the BG stays in the normal range around the clock (normal BG for the average cat is 70 – 120 mg/dL — yours might be higher or lower). Normalization is rarely attempted, because it means the cat is on the edge of hypoglycemia several hours a day, so what we do is “regulation” — holding the BG most of the time at levels which minimize harm to the cat. Your aim will be to keep the blood glucose above 100 all the time, and below 200 as much as possible.
If you want to control your cat’s diabetes as well as possible, buy a glucometer (any major pharmacy) and learn how to use it. Read the instructions until they are burned into your brain, and follow them to the letter. Practice sampling until it becomes a quick and easy process for both you and the cat — the cat will pick up on your mood if you’re having anxiety attacks about having to poke another hole in him. The first stick is the hardest, and after you’ve done ten you should be okay.
Many diabetic cat owners use the One Touch Ultra glucometer or the Therasense Freestyle. Both are easy to use and require only a very small blood sample. Glucometers have been improved a great deal lately, so make sure you have a fairly recent one. Usually you can find a glucometer that will be free, or nearly free, with a rebate.
Assorted Hints
- Never try to add blood to a test strip that seemed insufficient. The chemical reaction is an all-or-nothing deal
- Never repackage a test strip for later use after it’s been opened. They are extremely sensitive to humidity and substances that might be in the air.
- Never make insulin changes based on a single blood test reading. Use common sense and ask yourself if that reading was reasonable in light of insulin given, food given, the cat’s behavior, etc.
- Never do anything without having some idea in advance of what result you are expecting … subsequent decisions can then be based on whether or not you got the predicted result.
- Test strips are easily contaminated — wash your hands in case you wind up accidentally touching it, and don’t use it if it dropped on a dirty surface.
Insulin isn’t a drug like antibiotics or aspirin. It is a hormone (a substance produced in one part of the body which signals another part of the body to do something), and with its use you are attempting to mimic natural biochemistry, which varies considerably between individuals. Any insulin will work, but not necessarily very well in your individual cat.
Insulin is made from a number of sources, and some cats will do fine on human insulin and others better on a pork-sourced insulin, or beef a combination. All fluid insulins used in veterinary practice are mixed with substances that slow down their effect in the body. Natural insulin will start working in minutes, and be dispensed in tiny amounts according to how much glucose is entering the bloodstream. Injected insulin won’t start working for an hour or more (up to four), and will have it’s peak effect three to 12 hours after injection. It will disappear, whether or not it’s used for glucose uptake, anywhere from six to 36 hours after injection. The point at which it starts working is called the ONSET, the point at which it is working most strongly is called the PEAK, and the number of hours it works for is called the DURATION (together, these characteristics are called the ACTION PROFILE).
Manufacturers of veterinary insulins know the profile of their insulin for cats, and this information is packaged in every carton of insulin sold to vets. (If you get insulin from a pharmacy, they can look up the profile for humans and you can be guided by that initially.) You can determine the profile of your insulin through blood testing, but regulation is easier if you know in advance when to expect things to happen.
The insulin profile is tied to feeding. Insulin drives the blood glucose down, and food drives the blood glucose up. By monitoring blood glucose, you can know from hour to hour by which way the BG is going which of these is the stronger at that time. It’s a balancing act that eventually results in the two effects offsetting one another such that the blood glucose stays within your target range. The main trick is knowing when the insulin is having it’s strongest effect, and making sure that glucose from food is in the bloodstream at that time so it can be transported directly to the cells. The second trick is to make sure that no glucose (or as little as possible) is being put into the blood when there isn’t enough insulin action to cover it.
In the non-diabetic, the insulin is stopped when there is no signal to say it’s needed. With injected insulin, there is no such signal — once it’s injected and has started working, it will keep on working until something stops it or it breaks down. When the insulin is working, the BG is falling and the only thing that will stop the fall is putting more glucose into the system. The action profile will give you clues as to when it starts, when it’s peaking, and when it’s fading — you put food into the system to work with the peaks, and withold food during the tailing-off. Your blood testing will pinpoint the actual times in your cat, of the onset, peak, and fade. Regulation is the process of timing and quantifying the food into the insulin profile, and making small adjustments in both until they stabilize. It’s a pretty steep learning curve.
My approach to regulation with blood monitoring is two basic steps: first find the insulin dosage that gives you effectiveness, and then fine-tune the insulin and food until you have duration without compromising effectiveness. For this you have to make glucose curves and learn the meaning in them, and also be prepared to deal with an insulin reaction if it happens (these are discussed in separate sections). Do not trust your memory — it will get complex, and there will be many changes and many strange responses, so start a chart with plenty of room for wordy observations and questions.
Effectiveness
The starting point is always the vet’s recommended dosage and schedule. Do a baseline glucose curve and record the results. This means taking a blood test every hour or two (the interval should be regular, whichever you use) for a full insulin cycle (the time from one injection to the next, whether that is 12 or 24 hours). It doesn’t have to be completed in a single day — see ” Glucose Curves” below.
When you plot the BG readings over the number of hours in the cycle, plot the food, too. Pick out the time at which the BG was lowest on several consecutive days — say or example it turns out to be 3 hours … that’s the time of the insulin peak (not time of day, but hours post-injection). The degree of effectiveness your insulin and dosage are providing is revealed in how far it brought the BG down, not necessarily how close it came to normal range (although it’s lovely when the first dosage tried turns out to be the right one).
If the BG only came down a little and all the numbers are high, increase the dosage only — keep the frequency, and the food the same as it was for the baseline curve. Over the next few days, take blood tests at times that bracket the insulin peak — if the baseline curve says the insulin peaks at 3 hours, test at 2 hours, 3 hours, and 4 hours. As the BG approaches normal, the peak may start lasting longer and you must watch for this. It isn’t necessary to repeat the glucose curve again for a while, just monitor the peak.
If the insulin you’re using is formulated to have two peaks, you have to monitor both of them.
The size of the BG reading guides you in deciding how big an increase to make in the insulin dosage, and how many days to leave between dosage increases. The body takes from three to 14 days to “settle in” to a new insulin dosage, so the lower the BG gets the smaller the increases have to be, and the more days you leave between dosage changes.
If your baseline curve showed the lowest BG of the cycle was over 400 and the rest of the time it was much higher than that, be aggressive — for the next cycle (or the next day that you’re able to monitor), increase the dosage by a full unit, and bracket the insulin peak with blood tests again. If you find that the BG went lower this time, you’re on the right track, so do it again.
You must decide in advance when to switch from aggressive to conservative insulin increases, and when to cut back to fine-tuning. I suggest that when the lowest BG reading is 200-250, start making smaller increases (half a unit), and leave a minimum of three days between increases. You should see the lowest BG creep consistently downward. There should be noticeable improvement in behavior as well.
If you get curious and do blood tests at other times of the day while you’re working on achieving effectiveness, don’t be distracted by the readings you get. They may be all over the place, but you deal with them later. Right now you you just want to see that the BG drops significantly at some point in the cycle, and learn to control that drop.
Duration
When you get the lowest BG of the cycle down to 120-150, you have effectiveness. At this dosage, the cat is exposed to the risk of hypoglycemia if something goes wrong, so now your approach is permanently changed to one of caution — small changes, far apart, while you seek to improve the duration of the insulin action so the BG spikes stop.
When you’ve sustained effectiveness consistently for a week or two, do another full-cycle curve. For the first part of the cycle, monitor every two hours. After the peak has passsed, test every hour. When you plot the readings, you’ll be able to see how quickly the insulin tails off.
The good news is that if you lucked into the right insulin, the effective dose will also give you duration after a couple of weeks of settling-in. Your new curve will be very flat, with no big spikes at any point, and a gentle rise of BG in the last couple of hours of the cycle. If you get this, you’re done. Kitty is regulated!
If you don’t get this kind of duration, and the BG rose above 300, then you make small changes in feeding to extend the length of time the BG stays down (this is why you recorded feedings on the glucose curves). Do not make any changes to the insulin amount or times.
Reschedule your blood tests so that you’re doing a single test at the time of the insulin peak (just to make sure it doesn’t sink the BG too far). Look at the new curve to find the point at which the BG starts rising, and bracket that point the way you did the insulin peak before. As you make changes, you want to see that point moving closer and closer to the end of the cycle.
As with the insulin, the starting point for feeding changes is whatever the vet instructed you to do (see also the section on Feeding). If you don’t know how much food he is actually eating during an insulin cycle, take a couple of days and start measuring it.
Then you try to crowd all the food into the part of the cycle where the insulin is actually working, but only for the cycles when you can be there to watch. He should already be on an insulin/food scheme that works passably well, so for the cycles when you’re not home, stick with that until you know a stricter feeding schedule won’t get him into trouble when he’s alone.
When you are home, you can try scheduled feeding. A simple feeding schedule that sometimes works for a cat that isn’t overweight and not sharing his food dish with others is to just measure out more food than he needs at injection time and let him free-feed until the insulin peak has passed. Then pick up the dish and allow no more food until the next cycle. Measure whatever is left in the dish to calculate how much he ate and get an idea of what he thinks is enough food. (If your insulin has a slow onset, given only a tiny reward snack at injection time, then put down the measured food about an hour or two before the onset. If the onset is slow, the peak will be slow as well, so just leave the food down until the peak has passed.) After a while you may notice that he leaves more in the dish, and rations himself pretty effectively.
If his BG is still high part of the time and causing some PU/PD, he will also be extremely hungry and probably gobble it all down right away and either hurl it or have none left for the insulin peak. If he does this, go to plan B. Time the first meal to precede the insulin onset by an hour, and make it about 1/3 of the ration. The second meal, being the other 2/3 of the ration, is given to precede the insulin peak and stays available until the peak has passed. (If your insulin has a quick onset, give the first meal at injection time and the second one an hour before the peak).
If his insulin peaks while you’re asleep, you will have to change the time of his injections so the peak happens when you’re awake. Even if you never feel confident enough to use a timed feeding schedule when you’re away, at least you’ll have attained better duration for the night and weekend cycles.
Scheduled feeding is made more difficult by having other animals in the house, so how you accomplish it depends on you. Some people put all their pets on the diabetic’s schedule and slip extra food to the others. Some stand guard at mealtime to see that the right food goes down the right animal.
If you decide to free-feed around the clock, the only way you will regulate the cat is to just let him eat and provide enough insulin to cover what he’s eating. As the diabetes comes under control, he’ll be less urgent about food and his eating habits will change slowly until he reaches his personal equilibrium (which will probably involve gaining weight). If you choose this method, make your insulin adjustments very small — 1/4 to 1/2 unit, a week or two apart, and only make a change when you’re going to be home.
Monitoring the Regulated Cat
When the cat is regulated to your satisfaction, you get a big chunk of your life back. It is no longer be necessary to do complete curves. It is a good idea to spot-check occasionally — the time of the spot check doesn’t matter, as long as the reading fits his curve for that point in the cycle. Once or twice a week for the first couple of months is enough to assure you that he remains regulated, and once or twice a month after that. If you don’t like doing the ear sticks, now would be a good time to bring dipsticks into the picture, preferably testing before injection to ensure that the BG during the end of the previous cycle put only trace amounts of glucose the urine.
Many things will affect blood glucose temporarily, and if you get an out-of-range reading, don’t do anything about it. Simply note it, and try to identify the cause: he might have eaten less than usual; if it’s cold in the house he’ll be less active than usual; the shrieking toddlers that came to visit might have upset him; he might have a hairball; he might really hate those baths; the new vial of insulin might be stronger; the test might not have been accurate; some other medication (antibiotics prednisone, flea treatment) may be affecting the BG. Mostly it will be a one-time-only thing. If you’re really concerned, wait fifteeen minutes and test again.
If you suspect that the cat’s regulation has been lost, or have a reason to believe something is interfering with regulation, do a mini-curve and compare it to your last full curve. Test the blood glucose at these times:
- just before insulin is due, test for highest BG
- when the insulin is peaking, test for lowest BG
- when the insulin is starting to lose its effectiveness (one or two tests in the second half of the cycle to see whether the BG started rising sooner than before)
If the results are way off, and you can’t come up with an explanation, take the cat and all your data to the vet. There might be another disorder affecting the glucose levels.
Glucose Curve
The glucose curve will tell you if your cat responds as expected, or a little earlier, or later. It also tells if he’s responding enough, or too much.
For those who didn’t have the nerve to ask, it’s called a glucose curve because the results of the blood test readings (blood glucose levels, represented by g) are plotted on a graph over time, and when you connect the dots (g’s here) they make a curved line. It is an unmistakable picture of what is happening over the course of an insulin cycle. Here’s an example (this graph is only for for illustration).
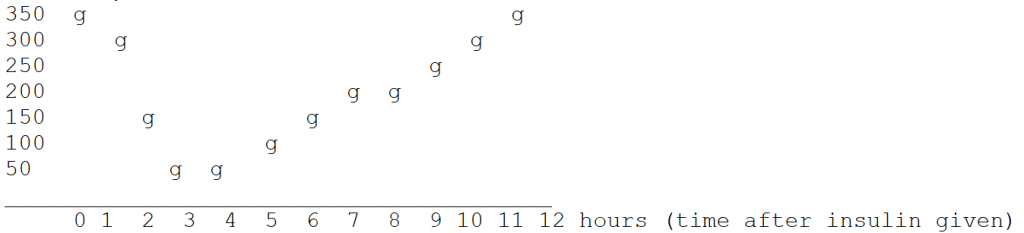
This curve illustrates effectiveness — at hour one, the BG is too high (350 in this example), then the BG starts coming down sharply when the insulin kicks in (onset before hour 2), insulin activity peaks (resulting in the lowest blood sugar level) at hour 3, holds the peak through hour 4, and starts rising back to the original level starting around hour 5. The duration isn’t good (i.e. glucose levels don’t stay in the normal range for long), the curve isn’t very flat, and the cat was seriously hypoglycemic (50 mg/dl) for hours 3 and 4.
By looking at the effects on the BG, you infer the action profile of the insulin, although you can’t plot it on the same graph because there are no numbers used to measure the strength of insulin action as it varies through the cycle. If it helps to conceptualize the action profile as a reverse curve, though, it would look like this where * is the value for the insulin action:
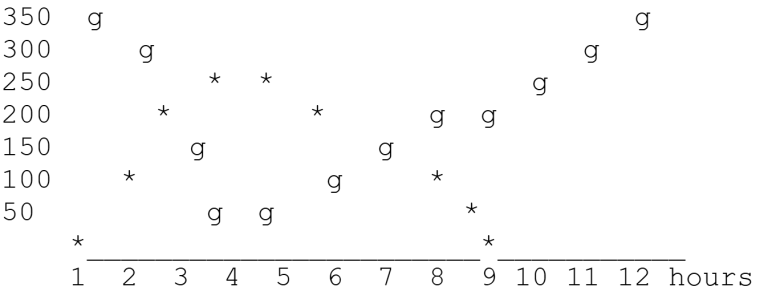
Note that the insulin curve is skewed to the left, with the action increasing quickly, hitting hard for a short time, and tailing off more slowly that it came on. Most insulins will skew in this direction, but some have later onsets and later peaks, and in some cats the tailing-off (or fading) will be more abrupt.
The curve gets more complex as you fit in the effects of feeding (represented by F on the graph). This one shows the same starting point and the same insulin action, but with food raising the BG at hour 2 before the onset of the insulin action. Also note that feeding prevents the hypoglycemia that showed in the graph above (the rise at hour 2 would have been much higher if the insulin hadn’t been working a little already).
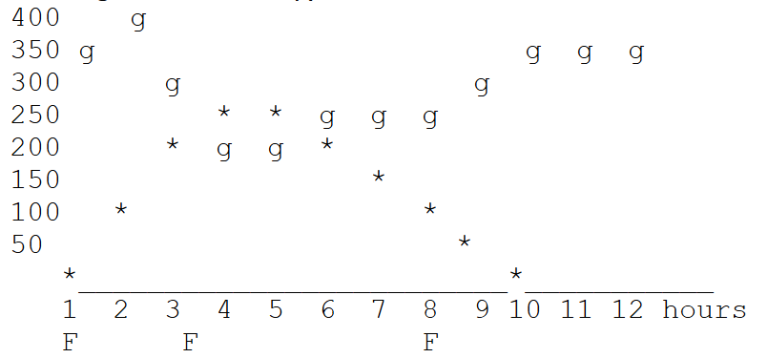
The third feeding, at hour 8, pushed the blood glucose up when the insulin action was fading, and the BG stayed high for the rest of the cycle.
The following curve shows the results over two cycles of insulin administration. In the first cycle, the BG is down for longer by eliminating the third feeding — for lack of new glucose, the blood levels stayed down when the insulin had faded. As a result, the next cycle has a lower BG starting point. The second curve is flatter. The rise after the first feeding is the same size, but a lower number, so when the insulin peaked the BG was right on target. The glucose was held down again after the insulin faded, but at a level below the previous cycle.
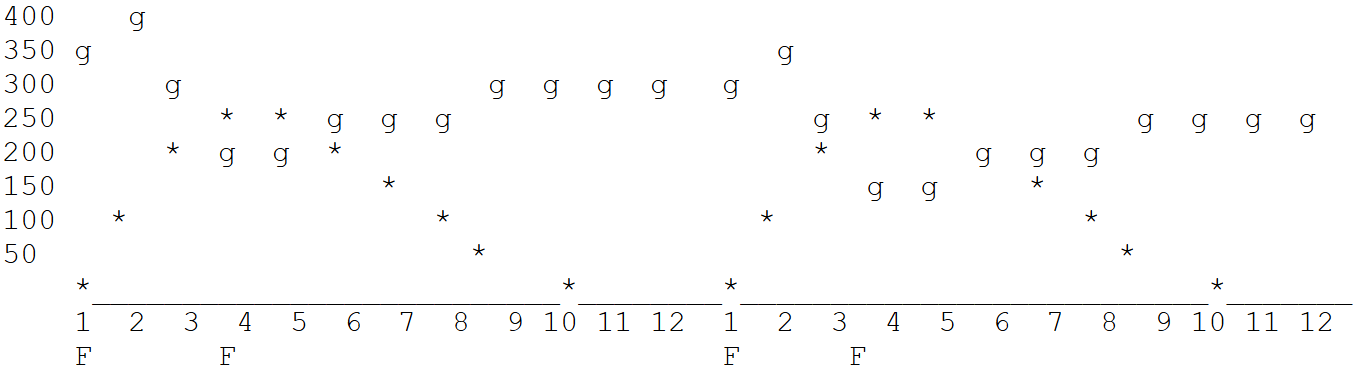
See how complicated it can get?
As the cat settles in and his system gets used to the insulin, you may even see the insulin overlapping — the next injection is due before the last one has completely faded away. This is fine, as long as the glucose readings remain within your target range.
Please do not look on these examples as curves you should attempt to get from your own cat — the numbers are entirely fabricated to illustrate the relationship of insulin and food over time. When you have a curve for your cat, study it and try to determine why it’s shaped the way it is. Your objective in regulating is to end up with the flattest possible curve, which never dips below normal, and if it rises much over 200 it should do so only briefly.
Normal blood glucose levels for the average cat are between 70 – 100 mg/dL) before a meal, and remain below 150 mg/dL after eating. An insulin-dependent cat’s optimal range would be thirty or so points higher overall, for safety.
Rarely, an animal will be extremely sensitive to low blood glucose and show signs of distress at 80 or more — if this is so for your cat, shift all the numbers upward for your particular circumstances.
Glucose curves done at the clinic may not establish the time of the insulin peak if your cat is on ultralente insulin — if they monitor him for six or eight hours, and the insulin doesn’t peak for 10 hours, the cat went through all that for nothing. To make this work, you might have to inject and feed several hours before taking him in for the all-day curve. Ultralente isn’t used much in cats, however.
Glucose curves don’t have to be done all in one day. If the insulin and food are held constant, you can spread the testing over several days and wind up with just as accurate a picture — possibly even more reliable than a day in which he got an ear stick every time he woke up. Also, you can start your curve at any time of day. For example, test at 7 pm and 9 pm Friday, 10 am and noon Saturday, and so on. When you have at least one test for every two-hour block, plot them all on one graph as if they were taken on a single day and in sequence.
Keep in mind that you did not have to interpret blood glucose curves. If you want to do the tests, plot the curves, and take them to your vet for interpretation (some will let you fax the curves), that is just fine.
More on Feeding
In the absence of Somogyi effect, food is the sole source of glucose going into the blood. Food and insulin must be balanced — just enough insulin to cover just that much food.
Some foods send blood sugar up very quickly, others are slower. None will last as long as the insulin does. Picky eaters can be a big problem — just remember that nutrition is the first criterion, so feed him whatever healthy food he’ll accept. If the cat is at his best weight, it is better to adjust insulin than food. Remember that his food needs will reduce as the diabetes comes under better control. When he regulates, he might even need a small insulin reduction after a while.
The nature of food affects the quantity and timing. Consistent amounts of consistent formulas provides the best diabetes control. In all foods, it is the carbohydrates and simple sugars that are converted to glucose. Simple sugars hit the bloodstream fast, the complex carbohydrates take longer because they have to be converted first. If you change your cat’s diet drastically, you should do at least a mini-curve to determine his response to the new food so you can adjust his insulin to cover it if necessary.
Fixed-formula foods are best, simply because the formulas are fixed — you know what’s in the bag every time you buy some. High-quality store brands will vary from batch to batch, but they generally stay within the parameters shown in the ingredients list. Don’t feed a diabetic cat bargain-basement foods … there’s no way of telling what they put in there, and the flavor usually comes from large quantities of fat and sometimes from sugars.
If he winds up gaining too much weight and you have to reduce his rations remember that you will have to cut back on the insulin as well to maintain regulation. Again, a mini-curve will guide you on how much to cut back. Carrying extra weight is bad for diabetics.
If the cat shows any signs of digestive upset (vomiting or diarrhea), you have to compensate. If they barf up their food occasionally, feed them again and watch to make sure it stayed down. If the cause is hairballs, ask your vet to recommend a treatment that doesn’t contain sugar or syrup or other things that will elevate BG. If you have to use a preparation that isn’t good for him, cut back on his food at the next meal to make up for the extra intake.
Treats are always a problem for diabetics. Whatever you give has to be considered part of their daily allotment, since even tiny amounts of food will have a significant effect on BG. If you have one of those trays that makes teensy tiny ice cubes, you can freeze the flavored water that we pour off of canned fish (but not if it’s oil) and melt one or two for a treat.
Ice cold food out of the fridge is hard on cat tummies, I’m told. I find it hard to nuke a tablespoon of food without vulcanizing it, so I warm up a heavy dish with water and then mash in the food to even out the temperature. I use glass ash trays — the shape lets them slurp the food out with reasonable efficiency, too.
If blood tests show the kidneys have been damaged, ask the vet for a reduced protein food even if it means compromising glucose control. Read the labels on everything you feed to check it’s protein content. Processing protein is harder on the kidneys than flushing a little glucose.
Hypoglycemia
Diabetes is a nasty disease that kills slowly. Insulin is wonderful stuff and saves countless lives. It works so well it can kill in hours, by reducing the blood glucose to zero.
Low blood sugar (hypoglycemia), if mild, causes little more than discomfort and hunger. When the BG level falls too far, you will see strange behavior, advancing to severe distress and possibly seizures, coma, and death. If there is vomiting at any stage of a hypoglycemic episode, suspect some other disorder that is upsetting the stomach — hypoglycemia shouldn’t happen if there’s still food in the stomach, unless it got there too late to be of help.
Some animals are very sensitive to even mild hypoglycemia, others give no obvious clues even when the levels are getting into what is generally thought to be dangerous territory. Sooner or later almost every cat goes hypo, so you have to be ready for it. Repeated severe episodes are damaging in themselves, resulting in vision, memory and other brain-related problems.
The only preparation you need for this is a bottle of corn syrup (e.g. KaroTM). You can keep glucose solution on hand, too, but any sugary substance will do, such as honey, pancake syrup, even table sugar dissolved in water. Corn syrup is effective, cheap, quite easy to administer, and keeps almost forever. One caution: keep the top of the bottle clean so the cap doesn’t get glued on — if it’s stuck shut while your cat is having an emergency your own anxiety levels will go through the roof.
There are a number of philosophies on how to deal with hypoglycemia. Some say load the cat with as much sugar as you can and take him to emergency. I use a less drastic approach,which doesn’t leave the cat with a huge glucose overload to deal with later. Keep in mind, however, that you must get the blood sugar levels up quickly and a brief period of hyperglycemia (blood sugar too high) is better than coma and death.
Should he go to the vet, or be left to recover? That depends on whether you can be there to watch for a few hours, and your own confidence levels. If you put three tablespoons of corn syrup into him, his BG levels will be through the roof for many hours, and exaggerated by the Somogyi effect which could last several days, so you might want the vet to handle that. If you were able to give just enough syrup to reverse the hypoglycemia and not raise his BG too high, you can do the follow-up at home.
The emergency will be over in half an hour, but he’ll need some follow-up attention, consisting primarily of observation and trying to decide whether he needs more food. how much, and for how long. The length of time you give follow-up feedings ought to be just for the length of time his insulin peak lasts — information you got from previous glucose curves. A blood test will tell you when his hypoglycemia is over, but if you don’t have a glucometer and he remains ravenous, give a small snack of his high-fiber food every hour or two until he calms down. (If you’re using a two-peak insulin, you may have to do follow-up feedings for several hours … if the first peak caused hypoglycemia, the second one may do it again.)
If the episode was serious and he passes out from exhaustion, wake him up every half hour for a couple of hours to check on whether he’s okay.
Do not change his insulin regime unless you’re certain the episode was caused by overdose. Check the food dish — he might have eaten less. Check the litter box for signs of diarrhea. Check around the house for vomit, in case he ate and brought it back up. If you find no evidence that a temporary shortage of food was the cause, you can cut back on the insulin by a half unit for three days. and watch him at peak time. If you can’t be there, cut back by a full unit. Don’t worry about spikes or PU/PD during those three days, since they’re probably caused by a temporary Somogyi rebound, but after that you want to do a mini-curve and make sure he went back to his regulated state.
1. MILD
While hypoglycemia is an emergency, you exercise some leeway in how you treat it. If the symptoms are mild (twitching, walking unsteadily, unusually urgent about being hungry), take a minute to think about the timing — if the insulin should be peaking around now, or you’ve changed the regime and the insulin peak time may be a bit early or late, then it’s probably hypoglycemia. If you have a glucometer, confirm your suspicions with a blood test (a urine test won’t help at all). A snack will bring the BG up again in a short time (probably half an hour). This snack should be some food that will get into the bloodstream faster than the high-fiber prescription foods — warm milk or cheese, Pounce treats, etc. Follow up as described above.
2. MODERATE
If the hypoglycemia hasn’t advanced too far, the cat will still have some control of his body — he might be too weak to stand, or is staggering or circling, huddling and trembly, disoriented, unable to see or correctly look in the direction of a noise. Immediately offer him a few drops of corn syrup, off a spoon or your finger — if he can’t lick it up, you have to get it into his mouth, but preferably not on his tongue (the sugar hits the bloodstream faster if absorbed through the lining of the mouth, so try and get the syrup on his gums and inside the cheeks … it’s thick and sticky, so this isn’t too hard). A syringe with no needle on it works if you aren’t willing to risk a finger.It doesn’t take much — four or five drops, and wait five or ten minutes. If he continues to get worse, don’t wait — give the same amount again. As soon as you see that his coordination is improving, give him a small snack of warm milk, cheese, cat treats, or whatever. In half an hour follow this with a small serving of his regular food, and then follow up as described above.
3. SEVERE
If you find your cat in an advanced state of hypoglycemia (collapsed or having seizures, bleeding from from the mouth, or comatose), make sure he’s on the floor in a fairly open space — if he has a convulsion before you get back with the syrup he could be injured. You do not have time to phone the vet, and the syrup bottle had better be exactly where you expect to find it when you’re half asleep and fully panicked.
Don’t try to restrain the seizures, but make sure he doesn’t hit up against something that could hurt him — just try to hold his head so you can stuff in at least half a teaspoon of syrup without choking him. Don’t fuss over over whether it’s on gums or cheek, just get it in there.
If you’re using your finger for the corn syrup, try not to get bitten. Kneel behind the cat and and hook the syrupy fingertip into the corner of his mouth, scraping the syrup off quickly into the corner of his lips. It’s messy, and a lot of the syrup will wind up on his face. Clean it off after he’s somewhat recovered, or he’ll end up ingesting it when it’s bad for him instead of good.
Over the next ten minutes, keep dabbing the syrup into his mouth, a drop or two every minute or so until he is recovered enough to eat. Then do follow-up feeding as in the last paragraph under “Moderate” above.
The last step is to clean off the top of the syrup bottle and put it back where it belongs.
Somogyi Effect (Rebound)
When a diabetic experiences hypoglycemia, the body tries to compensate. While it generally doesn’t have to, the liver is capable of producing glucose. The “signal” is glucagon, produced in the body in response to low blood sugar. Some vets treat hypoglycemia by injecting glucagon, which will keep the liver producing glucose for quite a while. The length of time it keeps putting out glucose is probably tied to the severity and/or duration of the hypoglycemia (or the size of the glucagon injection), but it can last 72 hours. The liver will generally kick in when BG levels get below 60, but in some it may happen at a higher level.
True Somogyi effect is quite rare in cats. Since they are obligate carnivores, their liver enzymes and glucose production ares different than that of humans and dogs.
Any hypoglycemic episode, whether or not you observed it, may be followed by some degree of rebound for some unknown length of time. It will show up as BG spikes happening before the insulin tails off, if you’re doing blood tests. If you’re using dipsticks, you’ll see a high reading at a time when you’re not even supposed to see traces. The spikes are almost as bad for the cat’s long term health as sustained high BG levels, so they should be stopped. Besides the other things damaged by high blood glucose, the poor old liver gets extra stress, and the long-suffering kidneys are thrown into overdrive again.
Unfortunately, the instinct is to increase insulin when we see high BG levels. If they are caused by rebound, the answer is to decrease insulin.
So how do you know whether to give more insulin or less? First you decide whether or not there is any possibility that hypoglycemia is occurring — if the cat is unregulated and never has a BG reading below 200, you’re probably not seeing rebound.
If hypoglycemia is an unconfirmed possibility, simply decrease the insulin by 20% for three days and see if the spikes disappear. Since food causes blood glucose to rise, it’s impossible to differentiate a Somogyi spike from a post-peak food spike — another argument in favor of restricted feeding.
Exercise
If the cat was seriously debilitated by the diabetes before it was brought under control, you’ll probably see a loss of function in the back legs. This is often thought to be diabetic neuropathy, when the high blood glucose has actually damaged the nerves. The diabetic experiences strange sensations from the damaged nerves, anything from numbness to excrutiating pain. Recovery is slow, and usually incomplete — it is certainly dependent on attaining optimum regulation of blood glucose levels.
The good news is the back leg weakness is often due to muscle wasting from extended disuse, and can be helped at home just by making the cat get some exercise. The bonus of this approach is that regular exercise reduces the need for insulin.
Exercise can be anything from gently tugging the legs so they use their muscles to pull away, or holding his favorite treats above a footstool or chair so they have something to lean on while they reach for the goodies. “Baby-walking” gives good stretches — hold up his front end and walk him between your feet so he has to take longish strides with only some of his weight on the weakened legs.
Miscellaneous
Cats are pretty tough creatures, and seem to resist the ravages of diabetes better than, say, dogs (who can go blind from cataracts in a matter of weeks if their BG isn’t controlled). They have a reputation for being extremely hard to regulate — many reports of insulin resistance, or temporarily revived pancreas functioning. Practically anything will throw them off track (a hairball or other digestive upset, physical or psychological stress).
Healing is always delayed in unregulated cats, but the better the regulation the better they heal or recover from other disorders. A really well regulated cat’s life will not be shortened significantly. It pays to have periodic blood tests done to see how the liver and kidneys are functioning, since both are intimately associated with glucose regulation.
When other problems arise, you’re stuck with a chicken-ang-egg dilemma. Some people are told not to try treating other illnesses until the diabetes is controlled — glucose is so fundamental to everything that happens in the body that no other single-organ disorder can possibly be treated with success if that is out of whack. On the other hand, how can the diabetes be well controlled if other problems are constantly throwing off the regulation? I go up the middle of the road, urgently treating all disorders and struggling to keep the BG regulated all the while.
Any loss of regulation that lasts more than a few days, or inability to achieve regulation, warrants a thorough checkup to see if something else is going on.
If you cat wears a collar, make sure the tag announces that he is diabetic and includes your phone number and/or the vet’s.
Steroids are really bad for diabetics, and large doses have actually induced diabetes in many animals.
Watch closely and learn the signs of early HYPERglycemia. This could be PU/PD or more nebulous signs. For Darlene’s cat, Pooter, one fairly reliable early sign of insufficient insulin is bloodshot eyes. Pull back the skin in front of the ear until you can see the whites of the eyes … if there are more veins than usual, or the white part is actually pink, check the BG levels.
Any illness that lasts more than a couple of days will probably necessitate an insulin reduction on the order of 10%. Sick cats eat less, move around less, and use less glucose. If he’s already sick, the illness will mask the signs of hypoglycemia. If vomiting is part of the illness, you may have to reduce the insulin as much as 50% to compensate for the reduced amount of food being digested.
Keep a close eye on diabetics with early kidney failure — if it worsens, the symptoms are PU/PD, the same as for diabetes out of control. You will need to have your vet check a BUN/Creatinine (pronounced B-U-N and referring to Blood Urea Nitrogen) periodically as a test of kidney function.
As an aid to those caretakers and cats facing a new diagnosis of diabetes, Darlene contributed an article in 1998 to help explain diabetes and what it entails. This article is based on that original article, although updated and altered considerably since that time. Thank you, Darlene.
This article is not comprehensive and it is not intended as an instruction manual. It attempts to personalize diabetes and to take away some of that fear we all face when first confronted with this disease.
If this article presents thoughts or data that you feel are incorrect or unclear, please feel free to start a discussion on the Feline Diabetes Message Board or email the webmaster.
Last updated October 2005.
